May 2, 2026
Varicose veins are enlarged, twisted veins that typically appear in the legs and feet when the valves inside the veins weaken or stop working properly. In a healthy circulatory system, veins carry blood back toward the heart using one-way valves that prevent backflow. When these valves become damaged or inefficient, blood can pool in the veins, causing them to stretch, bulge, and become visible under the skin.
This condition can develop slowly over time and may range from a mild cosmetic concern to a more significant medical issue that affects comfort and mobility. Some people notice small, visible veins at first, while others experience larger, rope-like veins accompanied by discomfort, aching, or heaviness in the legs. When symptoms begin to interfere with daily life or worsen over time, patients are often referred to vascular surgeons for further evaluation. These specialists focus on diagnosing and treating conditions that affect blood vessels and circulation throughout the body.
Exploring Causes of Vein Enlargement
Varicose veins develop when pressure builds inside the veins due to weakened or damaged valves. Instead of blood flowing smoothly back to the heart, it begins to flow backward and collect in the veins. This increased pressure causes the veins to stretch and enlarge over time.
Several factors can increase the risk of developing this condition. Genetics plays a major role, as individuals with a family history of vein disease are more likely to experience it themselves. Aging is another significant factor because vein walls and valves naturally weaken over time. Pregnancy can also contribute due to increased blood volume and hormonal changes that affect vein elasticity.
Lifestyle factors such as prolonged standing or sitting, obesity, and lack of movement can also increase pressure in the leg veins. Occupations that require long hours on the feet often contribute to the earlier development of symptoms. In more complex or advanced cases, vascular surgeons evaluate how blood is flowing through the venous system to determine the severity of the condition and whether deeper vein involvement is present.
Identifying Common Symptoms and Warning Signs
Symptoms of varicose veins vary depending on severity. Some individuals may only notice visible veins, while others experience discomfort such as aching, throbbing, burning, or a heavy sensation in the legs. These symptoms often worsen after long periods of standing or sitting and may improve when the legs are elevated.
Swelling around the ankles and lower legs is also common, especially later in the day. In some cases, the skin around affected veins may become dry, discolored, or irritated, indicating more advanced venous disease. When symptoms persist or begin to interfere with daily activities, vascular surgeons are often consulted to determine the underlying cause and evaluate whether treatment is necessary. Early assessment can help prevent progression and reduce the risk of complications.
Explaining Risk Factors and Condition Progression
Varicose veins develop due to a combination of genetic, physical, and lifestyle-related factors. A family history of vein disease significantly increases the likelihood of developing similar issues. Aging also contributes, as vein walls lose elasticity and valve strength over time.
Hormonal changes during pregnancy or menopause can also weaken vein function, making women more susceptible to developing varicose veins. Additionally, excess body weight places extra pressure on the lower extremity veins, increasing strain on the circulatory system. As the condition progresses, symptoms may become more frequent or severe. In some cases, individuals may develop chronic venous insufficiency, where blood flow is consistently impaired. Vascular surgeons assess the stage of progression to determine whether conservative care or medical intervention is appropriate.
Understanding Diagnosis and Evaluation Methods
Diagnosing varicose veins typically begins with a physical examination and a review of symptoms. A healthcare provider may examine visible veins while asking about discomfort, lifestyle habits, and family history of vein disease. This helps identify potential contributing factors.
In many cases, ultrasound imaging is used to evaluate blood flow and determine whether the valves in the veins are functioning properly. This noninvasive test allows specialists to see how blood is moving through the veins and whether there is any backward flow. When test results indicate more advanced venous insufficiency, vascular surgeons may be involved in developing a treatment plan. This ensures that both symptoms and underlying circulation problems are properly addressed.
Reviewing Treatment Options and Care Approaches
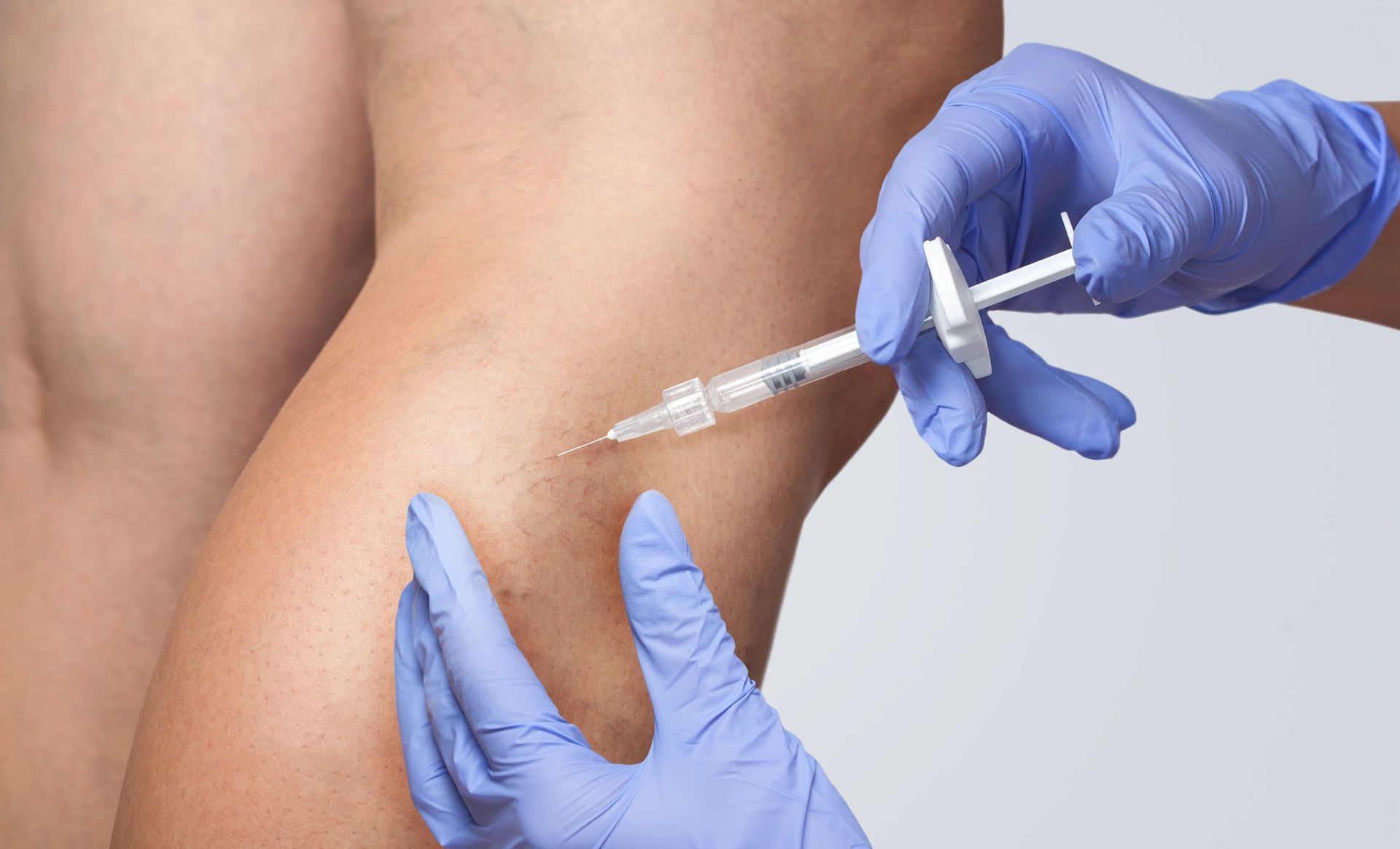
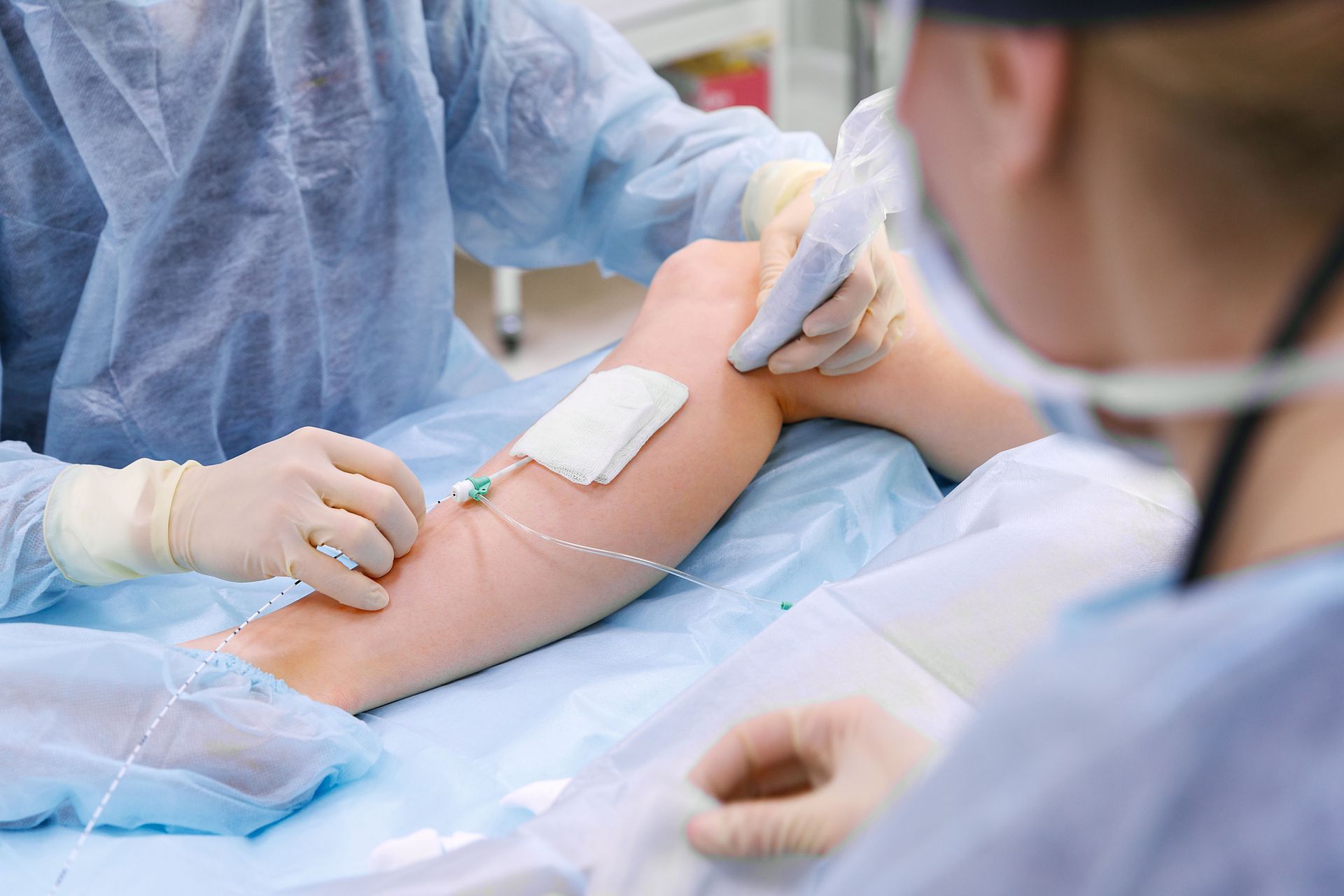
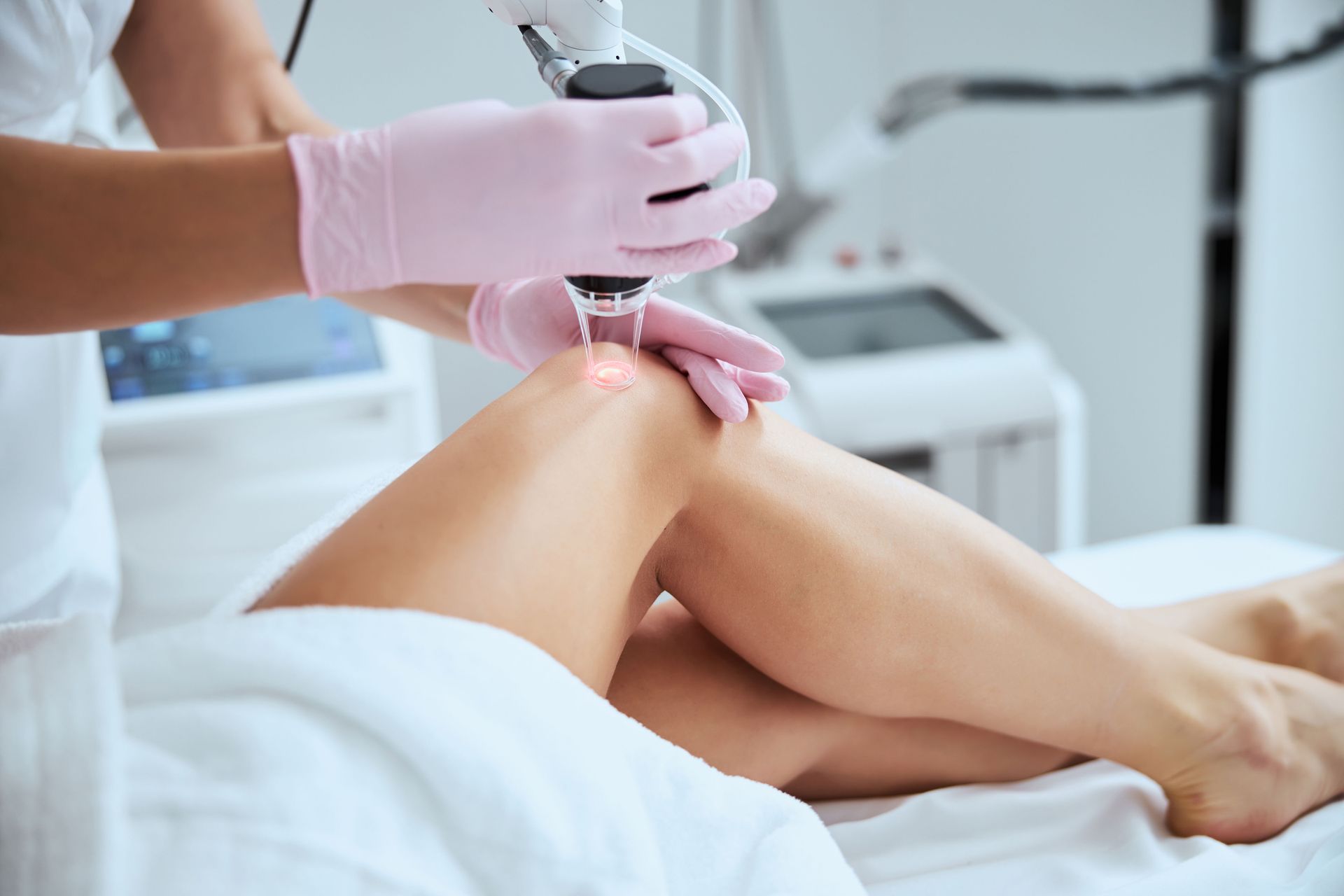
At Sun Vein & Vascular, we offer a range of treatments for varicose veins. These may include minimally invasive procedures such as sclerotherapy, radiofrequency ablation, and endovenous laser treatment. We also provide compression therapy and lifestyle recommendations. Our vascular specialists will create a customized treatment plan based on your specific condition, symptoms, and health goals.
Treatment options are designed to improve blood flow, reduce discomfort, and address both visible veins and underlying venous dysfunction. The appropriate approach depends on the severity of symptoms and how much the condition affects daily life. In some cases, conservative treatments such as compression stockings and lifestyle changes may be enough to manage symptoms. In more advanced situations, minimally invasive procedures may be recommended to close or remove damaged veins and redirect blood flow to healthier vessels.
Considering Lifestyle Changes and Prevention Strategies
While varicose veins cannot always be prevented, certain lifestyle changes can help reduce risk and slow progression. Regular exercise improves circulation and helps blood flow more efficiently through the veins. Activities such as walking, swimming, or cycling can be especially beneficial.
Maintaining a healthy weight also reduces pressure on the veins in the legs. Avoiding long periods of sitting or standing can help prevent blood from pooling in the lower extremities. Taking short breaks to move around or stretch throughout the day can make a noticeable difference.
Elevating the legs when resting can also help improve circulation and reduce swelling. Wearing supportive footwear and avoiding tight clothing around the waist or legs may further support vein health. When symptoms continue despite these changes, vascular surgeons may evaluate whether additional treatment is needed to improve circulation and prevent progression.
Recognizing When Medical Attention Is Needed
It is important to seek medical evaluation when varicose veins cause ongoing pain, swelling, skin changes, or interfere with daily activities. While some cases remain mild and manageable, others can progress into more serious venous conditions if left untreated. In advanced stages, complications such as skin ulcers, inflammation, or blood clots may occur.
These conditions require prompt medical attention to prevent further health risks and improve long-term outcomes. Vascular surgeons are trained to assess both the cosmetic and medical aspects of vein disease. They can determine whether treatment is necessary and recommend the most appropriate care plan based on each patient’s condition.
Understanding Prevalence and Health Impact
Varicose veins are a common vascular condition affecting a large portion of the adult population. According to the National Library of Medicine, around 24% of adults in the United States have visible varicose veins, and approximately 6% have evidence of advanced chronic venous disease. This highlights how widespread the condition is and emphasizes the importance of awareness and early evaluation. Although often viewed as a cosmetic issue, varicose veins can also indicate underlying circulatory problems that may require medical attention. Understanding prevalence helps normalize the condition and encourages individuals to seek care when symptoms arise.
Varicose veins develop gradually but can have a meaningful impact on comfort, appearance, and overall leg health. Understanding the causes, symptoms, and treatment options helps individuals take proactive steps toward better vascular health. Early diagnosis and appropriate care can reduce discomfort, prevent complications, and improve long-term quality of life.
With a wide range of treatment options available, most patients can find relief tailored to their specific needs. Sun Vein & Vascular is committed to providing comprehensive evaluation and advanced treatment options for varicose veins. Contact our team today to schedule a consultation and take the next step toward improved circulation, reduced symptoms, and better overall vein health.